Fast & Accurate Background Checks
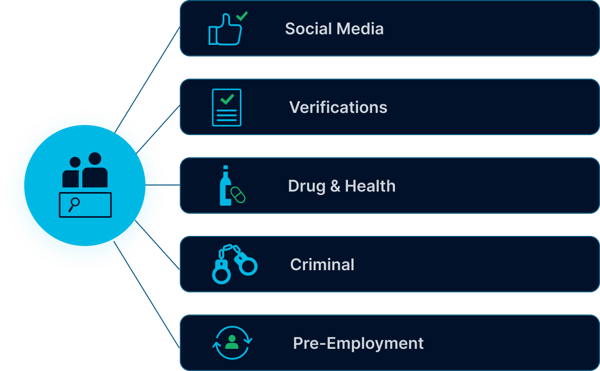


Why are Background Checks Important?
Today’s fast-paced hiring climate with streamlined applications and video interviews makes it challenging to weed out toxic candidates. But with a custom background check program, you can bypass the bad actors and focus on maintaining your company’s reputation.

Hire Better with Foley's Background Check Software
You need to hire fast. But you also need to hire well. Our background check programs help you do exactly that.

Pre-Employment Background Checks

Post-Hire Background Checks

Education & Employment Verifications

Personal Data Verifications

Social Media Monitoring

Criminal Background Checks

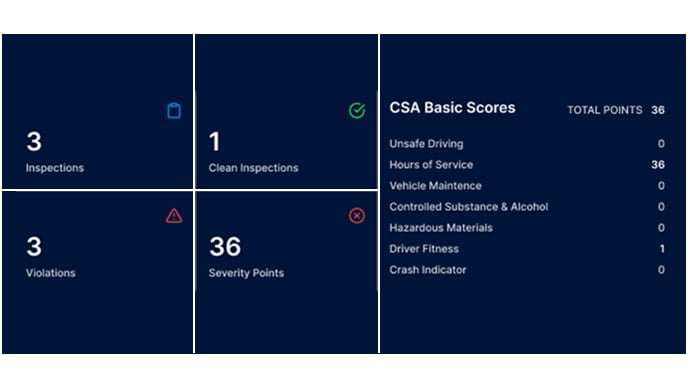
MVR Background Checks

Drug & Health Screenings


Informative Background Check Resources

What Shows Up in a Criminal Records Check?
Long considered the gold standard, "criminal history check" is what most people think of when they hear the words "background check." But how well do you know what criminal history checks cover? Get the facts!

Is this Legal? Social Media Background Check FAQs
How do you run compliant social media background checks? Hint: You can’t simply search a candidate’s profile. Find out how background check software for business runs these screens according to state and federal laws.
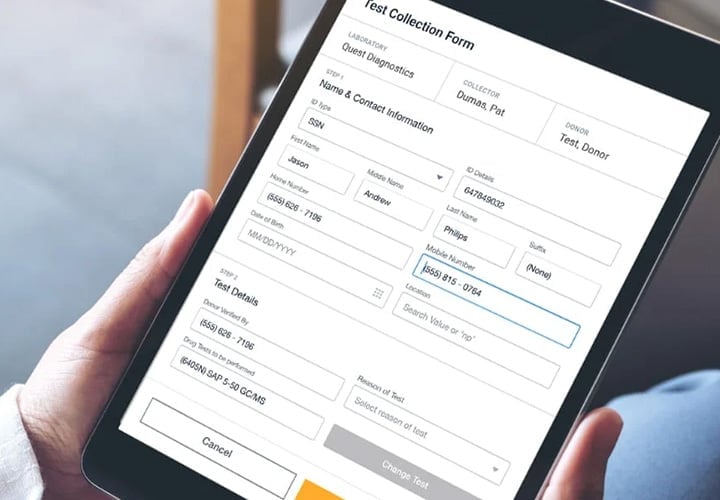
Understanding Panel Drug Tests – Expert Q&A
Drug testing is essential for pre-employment and employee screening. However, specific substance testing may be required based on job duties or regulatory requirements. Modern background checks demand a customizable panel.
.png)